BBC News, Русская служба - Главная
Главное

Live, Война в Украине: США выделили 6 млрд долларов на военную помощь Украине, в Киеве эвакуируются две больницы
Последние новости, комментарии и видео о войне России против Украины.

США отправят Украине помощь на $6 млрд. Это крупнейший пакет за все время войны, но новых «Патриотов» в нем нет
Министерство обороны США заявило, что купит у военной промышленности военное оборудование для Украины на общую сумму 6 млрд долларов. Это крупнейшая одиночная партия помощи, которую Вашингтон направит Киеву за все время российского вторжения, и в него включены ракеты для американских систем ПВО Patriot. Однако Пентагон не сообщает о выделении самих пусковых установок Patriot, о которых в последнее время просила Украина.

Франция получила Олимпийский огонь на церемонии в Афинах: фотографии
Олимпийский комитет Греции официально передал Франции огонь Летней Олимпиады 2024 года, которая пройдет в Париже с 26 июля по 11 августа.

Король Карл возвращается к публичной деятельности. Его лечение от рака проходит успешно
Король Великобритании Карл III на следующей неделе возвращается к публичной деятельности, сообщил официальный представитель Букингемского дворца.

Эмма Стоун хочет, чтобы люди называли ее настоящим именем
При рождении девочку назвали Эмили, и именно это имя актриса считает по-настоящему своим. Но по всему миру ее знают как Эмму.

«Разрушили все». Как российская оккупация навсегда изменила Чернобыльскую зону
Как изменилась Чернобыльская Зона за время войны в Украине.

Американские университеты сотрясают антиизраильские протесты. В Лос-Анджелесе отменена выпускная церемония, дошло до столкновений с полицией
Масштабные протесты против действий Израиля в Газе не стихают в кампусах американских университетов. Критики протестующих обвиняют тех в антисемитизме. Администрации университетов пытаются найти тонкую грань между свободой слова и экстремизмом.

Вашингтон призвал Пекин не содействовать России в войне, Китай предостерег США от пересечения «красных линий»
Министр иностранных дел КНР Ван И на встрече с госсекретарем США Энтони Блинкеном в пятницу в Пекине предостерег Вашингтон от пересечения «красных линий» в отношении Китая. А глава КНР Си Цзиньпин призвал США быть «партнерами, а не соперниками».

Двух британцев обвиняют в помощи российской разведке и организации поджога связанного с Украиной склада в Лондоне
Двум британцам официально предъявлены обвинения в содействии российским спецслужбам в связи с поджогом в Лондоне склада, принадлежащего компании выходцев из Украины.

Видео, «Все, что у меня есть, это мои руки, ноги и документы». Как новый закон о мобилизации затронул украинцев, живущих за границейПродолжительность, 4,31
23 апреля украинским мужчинам призывного возраста за рубежом временно перестали предоставлять консульские услуги. В паспортную службу Украины в Варшаве выстроилась очередь.
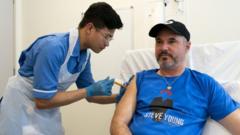
В Британии начались испытания первой в мире «индивидуальной» вакцины от меланомы
В Великобритании начались испытания первой в мире «индивидуальной» (то есть адаптированной под конкретного пациента) вакцины от меланомы — самой смертоносной формы рака кожи.

Лукашенко стал председателем ВНС; глава КГБ заявил, что по Минску хотели ударить дронами из Литвы. Главное в Беларуси за неделю
Русская служба Би-би-си рассказывает о главном в Беларуси за неделю
«Контекст» — рассылка, которая помогает понять новости
Подкасты
Не пропустите

Разочарованные в «своем государстве». Что не так с ограничением прав украинских мужчин за границей
23 апреля украинским мужчинам призывного возраста за рубежом временно перестали предоставлять консульские услуги, хотя положения нового закона о мобилизации вступают в силу только 18 мая. Как мужчинам за рубежом обновить данные в ТЦК, обязательно ли для этого ехать в Украину? А как в таком случае пройти медкомиссию? Украинская служба Би-би-си пыталась прояснить эти вопросы с юристами.

«Мы тебя выдаем России, только не плачь». Почему политэмигрантам опасно в Казахстане, Кыргызстане и Армении и кто помогает им уехать
Страны, куда можно въехать по российскому паспорту — Казахстан, Кыргызстан и Армения, — после начала войны в Украине стали центрами притяжения россиян, в отношении которых в России по политическим мотивам заведены уголовные дела. Эти страны сложно назвать безопасными для российских политэмигрантов из-за тесных связей с Россией и общей базы розыска.

«Круг насилия бесконечен». Защищают ли Женевские конвенции жертв современных войн?
Чуть ли не каждый день мы слышим, что кто-то нарушает Женевские конвенции. Но мы совсем не слышим, что кто-то понес ответственность за эти нарушения: ни судов, ни арестов — только сплошные выражения озабоченности. Не настало ли время задуматься о пересмотре этих конвенций, раз они не работают?

Звонил гадалке и переписывался со знакомой. Что делал экс-министр экономики Казахстана Бишимбаев, пока его супруга умирала в ресторане
В Астане продолжается суд над экс-министром экономики Куандыком Бишимбаевым, обвиняемом в истязании и убийстве своей супруги Салтанат Нукеновой.

Суд над Трампом по обвинению в выплатах порноактрисе Сторми Дэниелс: кто есть кто в уголовном деле экс-президента США?
В понедельник в Верховном суде штата Нью-Йорка начался суд над Дональдом Трампом, который продлится всю неделю. В рамках процесса экс-президент США отвечает на обвинения в выплатах порноактрисе Сторми Дэниелс, которые, по версии следствия, были призваны предотвратить распространение информации об их сексуальной связи.

Какой будет война в Украине и российское наступление летом 2024-го
Где ждать самых ожесточенных боев, и какая военная техника будет иметь решающее значение для каждой из сторон? Анализируем перспективы боевых действий и описываем общее развитие событий российско-украинской войны в ближайшие месяцы.

«Обязательный минимум» классической литературы: список книг от Габриэля Гарсии Маркеса
По случаю десятой годовщины со дня смерти Габриэля Гарсии Маркеса — единственного колумбийца, удостоенного Нобелевской премии по литературе — редактор испаноязычной службы Би-би-си Эрнандо Альварес делится списком классических произведений, составленных писателем по его просьбе, который он бережно хранит вот уже почти 30 лет.

Жесткая посадка Boeing. Что происходит с американским аэрокосмическим гигантом?
За последние годы с самолетами американского аэрокосмического гиганта Boeing произошло множество громких инцидентов, от просто неприятных до крупных катастроф. Почему компанию преследуют неудачи и допустят ли США банкротство Boeing?
События

В Хабаровске по делу о «фейках» об армии задержан журналист Forbes
Хабаровского журналиста Сергея Мингазова, работающего новостным редактором в российском издании Forbes, задержали по уголовному делу о «военных фейках». Поводом для дела стал репост в его личном телеграм-канале текста другого человека.

За граффити «Смерть режиму» школьницу из Читы приговорили к трем с половиной годам колонии
Первый Восточный окружной военный суд на выездном заседании приговорил читинскую десятиклассницу 17-летнюю Любовь Лизунову к трем с половиной годам колонии за граффити «Смерть режиму». Другие фигуранты дела Александр Снежков и Владислав Вишневский также осуждены.

Макрон: Европе грозит гибель, ей предстоит принять важные решения
Европа должна избавиться от своей добровольной наивности, в противном случае она ей может грозить гибель. Это суровое предупреждение легло в основу важной речи президента Франции Эммануэля Макрона о ЕС, с которой он выступил в четверг в Париже.

Дело замминистра обороны Тимура Иванова. Что известно об арестованных
Басманный суд Москвы 25 апреля арестовал третьего обвиняемого по делу о взятке, полученной, по версии следствия, заместителем министра обороны России Тимуром Ивановым и бизнесменом Сергеем Бородиным. Совладельца компании «Олимпситистрой», крупного подрядчика Минобороны Александра Фомина отправили в СИЗО.

Харви Вайнштейна будут судить снова. Суд отменил его приговор за изнасилования, вынесенный в 2020 году
Суд Нью-Йорка отменил приговор за изнасилования, вынесенный против голливудского магната Харви Вайнштейна в 2020 году, и назначил по этому делу новый суд.

Джулиани и другие соратники Трампа официально обвинены в попытке отменить результаты выборов президента США в Аризоне
Власти штата Аризона официально обвинили советника и адвоката Дональда Трампа Руди Джулиани, главу аппарата Белого дома при Трампе Марка Медоуза и еще 16 человек в заговоре с целью отменить итоги прошлых президентских выборов в этом штате. Сам Трамп числится в деле соучастником, но в число обвиняемых не включен.

Россия наложила вето на резолюцию ООН по предотвращению гонки вооружений в космосе
Москва утверждает, что и так выполняет Договор о космосе 1967 года и хочет полного запрета на размещение на орбите любых видов вооружений. США обвиняют Россию в разработке космического оружия.

Знаменитая ветряная мельница на кабаре «Мулен Руж» в Париже потеряла лопасти
Одна из главных туристических достопримечательностей Парижа — ветряная мельница над кабаре «Мулен Руж» на Монмартре — в ночь на четверг «потеряла» лопасти. По какой причине они обрушились и упали на мостовую, пока неясно.

Арестован замминистра обороны России Тимур Иванов. Что известно о нем и его деле
Басманный суд Москвы арестовал на два месяца заместителя министра обороны Тимура Иванова, которого накануне вечером, 23 апреля, задержали по подозрению в получении взятки.

Секреты папирусов Геркуланума: итальянский ученый нашел могилу Платона
Открытие удалось сделать благодаря расшифровке древних папирусов с помощью инфракрасной съемки и искусственного интеллекта.
Война России против Украины

Прорыв армии РФ у Очеретино в Донецкой области: чем это опасно для Украины
Пока украинские СМИ и соцсети выясняют, кто допустил беспрепятственный прорыв российских подразделений в село Очеретино к северо-западу от Авдеевки в Донецкой области, ситуация на этом участке фронта продолжает осложняться.

США тайно поставили Украине 300-километровые ракеты ATACMS. Их уже применили в Крыму
Соединенные Штаты в последние недели тайно поставили Украине ракеты 300-километрового радиуса действия ATACMS, и на прошлой неделе Украина впервые применила их в Крыму, сообщают американские чиновники и СМИ.

«Нас ждет тяжелый период, но Украина не проиграет». Интервью главы ГУР Кирилла Буданова Би-би-си
Кирилл Буданов — самый публичный руководитель военной разведки не только в истории Украины, но и в масштабах всего мира. Его прогнозы уже не такие оптимистичные, но, как утверждает он, Украина в войне, развязанной против нее Россией, не проиграет.

Не только через Тису. Украинец уплыл по Днепру на матраце в Беларусь, за что его осудили
В Беларуси судили украинца, незаконно переплывшего Днепр. Какими способами уклоняющиеся от мобилизации украинцы пытаются бежать из страны

«Это и есть Запорожская Сечь». Возродится ли Великий Луг на месте уничтоженной Каховской ГЭС
После уничтожения Каховской ГЭС, стоявшей на месте исторической части Запорожской сечи — Великого Луга, — многие опасались, что бывшее водохранилище превратится в пустыню или болото. Однако природа восстанавливается на удивление быстро, и властям предстоит решить, что с ней делать: восстанавливать ГЭС или превратить в заповедник.

Силовики пришли за продавцом шевронов для силовиков. Как волонтер и сотрудник парка «Патриот» стал обвиняемым в госизмене
Фигурантом нового дела о госизмене стал волонтер прокремлевского движения «Мы вместе», узнала Би-би-си. 26-летний Николай Мартынов во время войны с Украиной работал инженером в парке Минобороны «Патриот» и продавал шевроны с символикой силовиков. До ареста по «шпионской статье» суды пять раз подряд отправляли Мартынова в спецприемники — он провел там больше двух месяцев за якобы «нецензурную брань» и «неповиновение полиции».

Расследование Би-би-си: сколько может выжить на фронте в Украине российский заключенный?
За последний год заключенные, уехавшие на фронт из российских тюрем, принимали участие во всех ключевых боях на войне в Украине. Изучив истории более 9 тысяч отправленных на фронт осужденных, Би-би-си постаралась выяснить, как долго им удается выжить на войне и меняется ли этот показатель со временем.

Словаки в пику премьеру Фицо собрали 3 млн евро на снаряды для Украины
Граждане Словакии, недовольные отношением правительства Роберта Фицо к Украине, объявили сбор средств на закупку снарядов для украинской армии — и уже в первые двое суток собрали больше, чем планировали

Российские потери в Украине к апрелю: 51 тысяч подтверждено, средние потери за неделю остаются выше, чем в 2022 году
На основе открытых источников Би-би-си совместно с изданием «Медиазона» (признано в России «иноагентом») и командой волонтеров удалось установить имена 51 096 российских военных, погибших на войне в Украине с февраля 2022 года. По меньшей мере 43% не были связаны с армией на момент начала вторжения в Украину.

«Такая двоякая ситуация». Как мать-одиночка из Сибири решила перевоспитать уголовника из ЧВК «Вагнер»
В России к обычной жизни стали возвращаться наемники ЧВК «Вагнер» — бывшие заключенные, помилованные Путиным в обмен на участие в войне в Украине, в том числе осужденные за тяжкие насильственные преступления. Би-би-си рассказывает, как жительница Красноярского края решила перевоспитать незнакомого ей ранее экс-наемника ЧВК «Вагнер».